PICU Guest Lecture
by Dr. Weinerman. Clinician, Professor, and Clinical Informatician. Works with Dr. Soojin Park.
Pediatrics lags behind in ressearch compared to adults (30 years mentioned!). HR of 1yo is different than 2yo. They are not small adults! Most treatments are weight based (Baby meds are in mcg/kg/min.) Kids cannot tell/give feedback.
PICU is a relatively new field. Most of this came around during Polio (how you ventilate an adult is different than how you ventilate a child.)
Adult ICU — Mortality 30-35%. In PICU is 1-2%! Keep morbidity in mind though.
41 Bed unit at Columbia with 3 ICUs (neuro critical care, cardiac PICU, generic (asthma pneumonia liver xplt) ICU). 2000 admissions p.a. (500 cardiac).
They treat people from their birth to their teen years who are critically ill. Unstable life-threatening conditions, and at risk for organ failure.
Who comes in to ICU? Closer monitoring (1 nurse → 4 patients, versus 2 in ICU)
- Unstable hemodynamics (shock, bleeding, resp failure).
- ECMO (do the work of the heart and lung) CRRT (do work of the kidneys) VADs (pumps blood out of heart for them) are only found in ICUs.
- Potent vasoactive medications (epi, insulin, anti coag).
- At risk for clinical decompensation (airway, agitation, bleeding, neurologic monitoring).
Post Scoliosis corrections/surgereis in children are monitored in ICU. 99% are successful but a lot of things can go wrong.
When a baby is born she goes to the NICU. When the child is discharted, they are considered “dirty” exposed to the world. THen if they are readmitted they go to the PICU. In general, a baby only ever enters a NICU once (exceptions are ok).
Top 10 problems (17%): Hypoxia, Resp disease, fever, tetralogy of fallot, hypoplastic left heart syndrome, seizure…
Top 10 coded diagnosis: Tetralogy of Fallot, Sepsis, Acute bronchiolotis due to RSV, ventricular septal defect, Acute bronchiolotis due to other, hypoplastic left heart syndrome, idiopathic scoliosis, acute and chronic resp. failure, status asthmaticus, acute respiratory failure.
Tetralogy of Fallot — constellation of 4 problems in the heart.
Discussion on intestinal transplant. Very low chance of success (Columbia is one of the few places that does this; intestines, liver, pancreas.) Your body attacks the new organs so any transplant needs immunosuppression. The gut is one of the most infested part of your body…
People Involved
- PICU Attending
- PICU Fellow
- Front Line Provider — Person putting in the orders and helping to manage the patient. You’re the ‘fixer’/manager sort of. Can be a resident or NP or PA. Overseen by fellow.
- Nurses
- Case Managers — Looks at things outside of the hospital.
- LISW
- Consultants
- Nutritionist
- Pharmacist
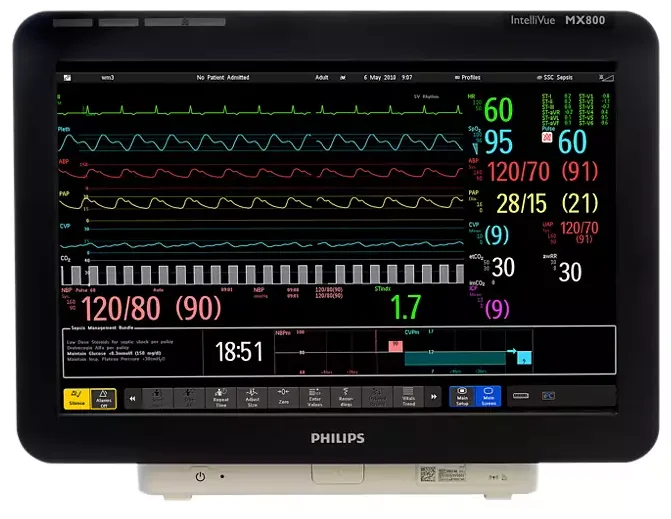
At least in the ICUs, Columbia stores all these numbers for ~15 years or so. E.g. Telemetry for EKG is @512Hz sampling rate! 1.97 million data points per hour! Plethmography is 200Hz, CO_2 is 1Hz, arterial is 200Hz, etc. Note that NYP owns all this data.
This stuff requires IRBs. See open waveforms like Stanford Waves.
Clinical Workflow
Home → ED → Labs → OR or Hospital/ICU
Home → OR → ICU
Floor → Deterioration → ICU
You use a “gas sheet” for various gases (VBG - venous blood gas, ABG) in the blood through blood draws. Babies you can use the heels because they haven’t walked and they’re very vascular! This is a capillary blood draw.
Patient -> Lab -> EHR
-> Documentation (Nurses, Attending) -> EHR
-> Machines -> EHR
Problem is a lot of cross-talk. Which source do you trust?
Data
First two are a big majority of EHR data!
- Flow Sheet Data — Check on the patient and log things. Nurse can put these into a column themselves. Or a machine (like ECMO) can do this but a nurse has to initiate this. Like what if you’re doing cartwheels and your HR is high? This is done at the nurse’s discretion.
- Lab Data — What it says.
- Monitor Data — This is from the real-time data. A nurse can choose to turn this into Flow Sheet Data.
Cardiac Index
To normalize, you divide by Body Surface Area.
This is Cardiac Index. No gold standard method to get this non-invasively at bedside!
Really Random
- Sometimes you can contact a rehab center to help parents move their arms, make sure they are comforable with taking masks on and off, etc… this is outside of the hospital; insurance is involved.
- Imagine giving a baby a chest patting so they clear chest secretions. Imagine what this does to the EKG readings. Now imagine that the EKG going haywire might indicate that there was a patting going on… oh data!
What classifies as pediatrics? Question is what do you see? Do you see adult physiology and pathology? Then they might be underserved at a pediatrics unit. Babies don’t smoke drink fatty foods and clogged arteries — what do you see? Would they be Underserved in an adult clinic? People would like to transition you to an adult provider to take care of your care (usually > 20).
Sickle cell — transition to adult hematologists.
Funding is a problem in Pediatric research and care. Majority of cases, kids get better. What about the rest?
Newborn heart is the size of a walnut 🥲
BTT shunt. Was called BT shunt because a T in there was Black and left off (of course.)